Alcohol detox is not just uncomfortable. For many people, it is genuinely life-threatening, and understanding what is alcohol detox danger signs Texas residents need to recognize could be the difference between survival and a medical emergency. The reality is that most people who attempt to stop drinking on their own do not realize how fast withdrawal can turn dangerous. Seizures, hallucinations, and a condition called delirium tremens can develop within hours of the last drink. If you or someone you care about is in Texas and considering stopping alcohol use, this guide will give you the medical facts, the warning signs to watch for, and the local resources available to help.
Table of Contents
- Key takeaways
- Understanding alcohol withdrawal symptoms and timeline
- Recognizing alcohol detox danger signs in Texas
- Why medically supervised detox is essential
- Texas alcohol treatment options and support resources
- My perspective on detox awareness in Texas
- Safe detox in Texas starts with the right support
- FAQ
Key takeaways
| Point | Details |
|---|---|
| Withdrawal starts fast | Symptoms can begin within 6 to 12 hours of the last drink, escalating rapidly. |
| Delirium tremens is deadly without care | Untreated DTs carry a 15 to 20% mortality rate, reduced to under 1% with medical treatment. |
| Certain people face higher risk | Heavy daily drinkers, those over 50, and anyone with prior seizures face the most danger. |
| Medical supervision is non-negotiable | Benzodiazepines administered by physicians reduce seizure risk by over 90%. |
| Texas has crisis resources | Call 988 for substance use emergencies or 911 for life-threatening symptoms like seizures. |
Understanding alcohol withdrawal symptoms and timeline
Alcohol withdrawal is a physiological response. When someone who drinks heavily stops suddenly, the central nervous system, which has adapted to the constant presence of alcohol, goes into overdrive. The result is a cascade of symptoms that can range from mild discomfort to a life-threatening crisis.
Withdrawal symptoms range from mild anxiety and headache all the way to hallucinations and seizures, progressing in stages over a period of days. Understanding that timeline is critical because the window for the most dangerous complications is narrow and specific.
Here is how the typical progression unfolds:
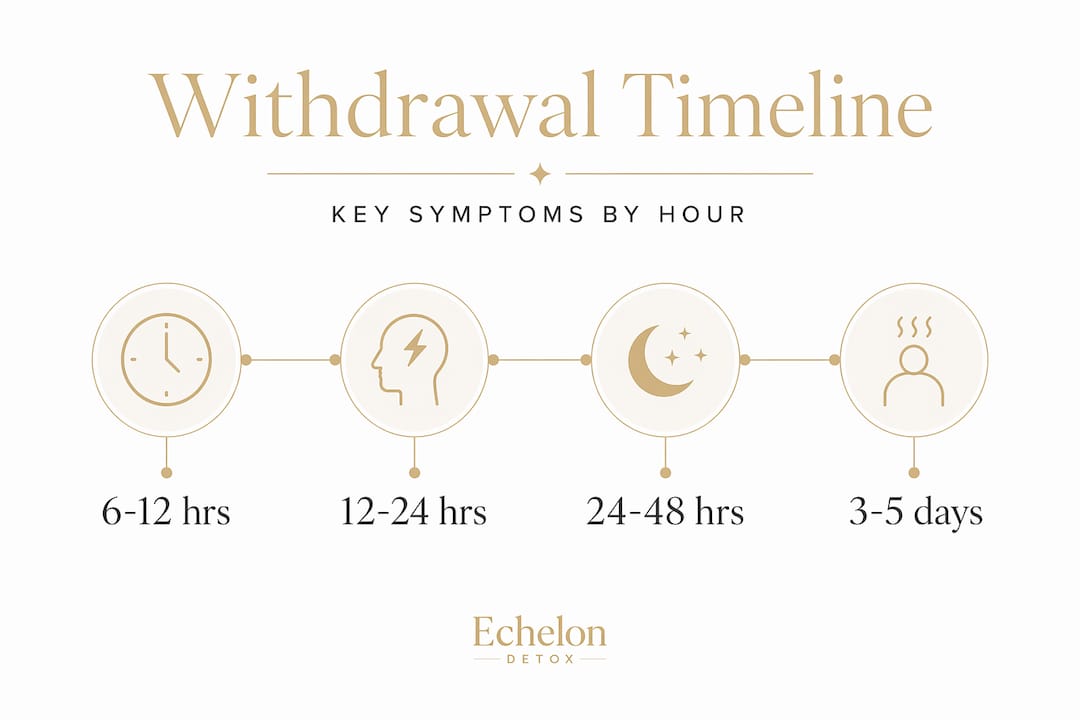
- 6 to 12 hours after the last drink: Early symptoms appear. These include anxiety, restlessness, hand tremors, nausea, vomiting, headache, and elevated heart rate. Many people mistake this stage for a bad hangover.
- 12 to 24 hours: Withdrawal hallucinations may begin. These are typically visual or auditory and occur in roughly 25% of people experiencing withdrawal. The person may see or hear things that are not there, even while remaining conscious and oriented.
- 24 to 48 hours: This is the peak seizure risk window. Generalized tonic-clonic seizures can occur without warning. A person can be walking around, appearing relatively stable, and then experience a seizure with no prior indication.
- 48 to 72 hours: Delirium tremens, commonly called DTs, can develop during this period. This is the most severe form of alcohol withdrawal and constitutes a full medical emergency.
The timeline varies based on individual factors. Someone who has been drinking heavily for decades will not follow the same pattern as someone who has been drinking heavily for two years. Severity of withdrawal is highly individual and tied to the duration of heavy use and prior withdrawal history, which is exactly why a one-size-fits-all approach to detox is so dangerous.
Pro Tip: If you or someone you know has ever experienced a seizure during a previous attempt to stop drinking, the risk of another seizure during the next withdrawal is significantly higher. This is not a situation to manage at home.
Recognizing alcohol detox danger signs in Texas
Knowing the difference between uncomfortable withdrawal and a medical emergency is something many people in Texas are not prepared for. The alcohol detox danger signs that require immediate action are specific, and recognizing them quickly matters enormously.
The following are the warning signs that signal a genuine emergency:
- Seizures. Any seizure activity during withdrawal is a medical emergency. Call 911 immediately. Do not wait to see if it passes.
- Hallucinations. Seeing, hearing, or feeling things that are not real, especially when combined with confusion, indicates the nervous system is in serious distress.
- Severe confusion or disorientation. If a person cannot tell you where they are, what day it is, or who you are, this is a red flag for delirium tremens.
- High fever. A temperature above 100.4°F during withdrawal is a clinical warning sign associated with delirium tremens, which involves autonomic hyperactivity including hyperthermia and hypertension requiring ICU-level care.
- Rapid or irregular heart rate. A racing or irregular heartbeat during withdrawal can indicate dangerous cardiovascular stress.
- Severe agitation or uncontrollable shaking. When tremors become whole-body and the person cannot be calmed, this goes beyond typical withdrawal discomfort.
Certain people face a much higher risk of experiencing these severe complications. High-risk predictors include heavy daily drinking, being over age 50, a history of prior withdrawal seizures or DTs, co-occurring medical illnesses, dehydration, and poor nutrition. If any of these factors apply to you or someone you love, the risk of a severe withdrawal event is substantially elevated.
"Alcohol withdrawal is a medical emergency for many, not merely flu-like discomfort. Professional supervision is critical to safely navigate early recovery's most volatile hours." — Medical experts in substance use care
For Texans specifically, there are two numbers worth knowing right now. The 988 crisis lifeline operates 24 hours a day, 7 days a week, and handles substance use emergencies in addition to mental health crises. OSAR programs, which stands for Outreach, Screening, Assessment, and Referral, connect individuals across Texas to state-funded withdrawal management services. For any life-threatening symptom, call 911 without hesitation.
Why medically supervised detox is essential

The appeal of detoxing at home is understandable. It feels private, familiar, and less intimidating than entering a clinical setting. But home detox carries serious risks because severe symptoms can escalate rapidly and without warning, and there is no way to manage a seizure or delirium tremens without medical support.
Here is a direct comparison of what home detox versus medically supervised detox actually looks like in practice:
| Factor | Home detox | Medically supervised detox |
|---|---|---|
| Seizure management | No capacity to respond | Medications and trained staff on hand |
| Medication access | None | Benzodiazepines reduce seizure risk by over 90% |
| Vital sign monitoring | None | Continuous monitoring of heart rate, BP, temperature |
| Delirium tremens response | No intervention possible | ICU-level protocols available |
| Nutritional support | Self-managed | Thiamine supplementation to prevent neurological damage |
| Outcome | Unpredictable and high risk | Significantly safer with lower mortality |
Benzodiazepines are the standard medical treatment for alcohol withdrawal, decreasing seizure risk by over 90% when administered appropriately. These medications are not available without a physician, which is one of the clearest reasons why attempting detox without medical oversight is genuinely dangerous.
Beyond seizure prevention, inpatient monitoring includes vital sign checks, hydration management, and vitamin supplementation, particularly thiamine (Vitamin B1), to prevent Wernicke-Korsakoff syndrome. This is a serious neurological condition that develops in chronic heavy drinkers due to thiamine deficiency and can cause permanent memory damage if not addressed during detox. It is frequently overlooked in home settings.
Pro Tip: If you are considering stopping alcohol use and you drink daily or have been drinking heavily for more than a few months, speak with a physician before your last drink, not after. Planning ahead gives medical professionals the ability to prepare a protocol that keeps you safe from the very first hour.
Understanding why medical oversight matters during detox is not about fear. It is about giving yourself the best possible chance at a safe start to recovery.
Texas alcohol treatment options and support resources
Texas has a network of resources designed to help individuals access safe detox, and knowing where to turn before a crisis develops can save your life or the life of someone you care about.
Here is where to start if you or someone you know needs help right now:
- Call 988. The Suicide and Crisis Lifeline now covers substance use emergencies in Texas. Trained counselors are available 24 hours a day and can connect you to local withdrawal management services without judgment.
- Contact your local OSAR program. Outreach, Screening, Assessment, and Referral services operate across Texas and coordinate access to state-funded detox and withdrawal management programs. They can help you find the right level of care based on your specific situation.
- Go to the emergency room. If symptoms are severe, including any seizure activity, severe confusion, high fever, or chest pain, do not wait. Go directly to the nearest emergency room or call 911. Texas emergency departments are equipped to manage acute alcohol withdrawal.
- Reach out to a private detox provider. For individuals who need medically supervised care with privacy and personalized attention, private concierge detox services offer physician-guided support in a confidential setting.
- Talk to your primary care physician. If you have a doctor you trust, they can assess your withdrawal risk level and refer you to the appropriate level of care before symptoms begin.
The most important thing to understand about Texas alcohol treatment options is that early contact with any of these resources dramatically improves outcomes. Waiting until symptoms become severe narrows the window for effective intervention. Reaching out before the last drink, or at the very first sign of withdrawal, is always the right call.
My perspective on detox awareness in Texas
I have seen the pattern repeat more times than I can count. Someone decides they are ready to stop drinking, they tell themselves they will push through the discomfort, and they underestimate what their body is about to go through. Sometimes that works out. Often, it does not.
What I have learned is that the people most at risk are frequently the ones who feel most confident about managing it alone. They have been through withdrawal before. They know what to expect. But what they do not always account for is that each withdrawal episode can be more severe than the last. That is not a scare tactic. That is neuroscience.
In my experience, the awareness gap in Texas is real. People know about rehab. They know about AA. What they are less clear on is that the first 72 hours of stopping alcohol use can be the most medically dangerous period of their entire recovery. Knowing the alcohol detox warning signs and having a plan before that window opens is not optional for high-risk individuals. It is the foundation of staying alive long enough to actually recover.
Medical detox is not the cure. It is the starting point. But without it, many people never get the chance to take the next step. Texas has resources, and more are becoming available. The challenge is that awareness still lags behind the need. If reading this prompts one person to call 988 or reach out to a physician before attempting to stop drinking alone, that matters.
— Nichol
Safe detox in Texas starts with the right support
If you recognize yourself or someone you love in what you have read here, the most important next step is reaching out to a team that can provide real medical oversight, not just encouragement.
Echelondetox provides physician-guided, 24/7 in-home detox care for individuals across Texas who need medically supervised support with complete privacy. Every plan is built around your specific health history, risk factors, and personal needs. Licensed physicians and nurses manage your withdrawal from the first hour, with access to the medications and monitoring that make detox genuinely safe. You do not have to choose between your privacy and your safety. Visit Echelondetox to learn more or speak with a care coordinator today.
FAQ
What are the most dangerous alcohol detox signs?
The most dangerous alcohol detox warning signs include seizures, severe confusion, high fever, rapid or irregular heartbeat, and hallucinations. These symptoms, particularly when they occur together, indicate delirium tremens, which requires immediate emergency medical care.
When do alcohol withdrawal symptoms start?
Alcohol withdrawal symptoms typically begin 6 to 12 hours after the last drink, with seizure risk peaking between 24 and 48 hours and delirium tremens developing between 48 and 72 hours after stopping alcohol use.
Is it safe to detox from alcohol at home in Texas?
Detoxing from alcohol at home carries serious risks, including the possibility of unmanaged seizures and fatal delirium tremens. Medically supervised detox with physician oversight and access to medications like benzodiazepines is significantly safer for anyone with a history of heavy or prolonged alcohol use.
Who is at highest risk during alcohol withdrawal?
High-risk individuals include those with a history of prior withdrawal seizures or DTs, heavy daily drinkers, people over age 50, and those with co-occurring medical conditions. These individuals should seek inpatient or medically supervised detox rather than attempting to stop drinking without professional support.
How do I access alcohol detox help in Texas?
Call 988 for immediate substance use crisis support available 24/7 across Texas, contact your local OSAR program for state-funded withdrawal management referrals, or go to the nearest emergency room if symptoms are severe. Private physician-guided detox services are also available for those who need confidential, personalized care.
